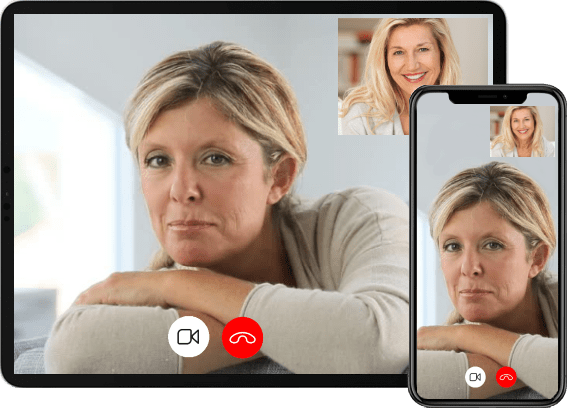
Why Choose the Virtual Therapist Network for Online Therapy?
Convenience
Daily life is busy. Add work or school, errands, children, travel time and the cost of gas to your therapist's office and therapy becomes inconvenient at best. Online therapy lets you do it all from the comfort
of your home and within your schedule.
Comprehensive
With online therapist search, messaging,
My Network, appointment scheduling, and video/audio sessions, we provide everything you need for a successful online therapy meeting with your chosen therapist.
Affordability
Since 2014, the cost to use VTN for online therapy has not changed. At only $4.95 per month, we still offer the most affordable membership available.
Comfort
Apprehensive about therapy? Maybe you're suffering from anxiety or agoraphobia that’s holding you back. Or, maybe you're just worried about running into someone you know. With online therapy, you can take your sessions in the comfort of your own home and never have to worry about those things.
HIPAA Secure
Using both SSL and TSL for all text, video, and audio communications with your online therapist means you don’t have to worry about your online therapy privacy.
Anonymity
We respect your right to privacy and anonymity. For that reason, we keep membership information to a bare minimum and only ask for the information needed to create your account and facilitate a meeting with your selected provider.
How it Works?
Register
Search for an Online Therapist
or Counselor
or Counselor
Book an Online Therapy
Appointment
Appointment
Login and Enter Conference
Room
Room
What is the Issue You're Needing Help with?
Select an issue you're having trouble with and we'll show you online therapists and counselors who can help.
Are You a Provider?
6 Reasons Why Independent Therapists, Counselors, & Life Coaches Join the Virtual Therapist Network

HIPAA Compliant

BAA Included

Flexibility

Appointment Calendar

MHR Client Charting

Affordability